Written by Laurie Ray, MPT, PhD, who has over 18 years of experience in school-based practice and is a state-level PT consultant for public schools. She also consults for Medicaid and Adapted Physical Education for her state and is an Associate Professor at UNC-Chapel Hill. Laurie also teaches continuing education via Apply EBP. More about these courses after the article below.
[smbtoolbar]
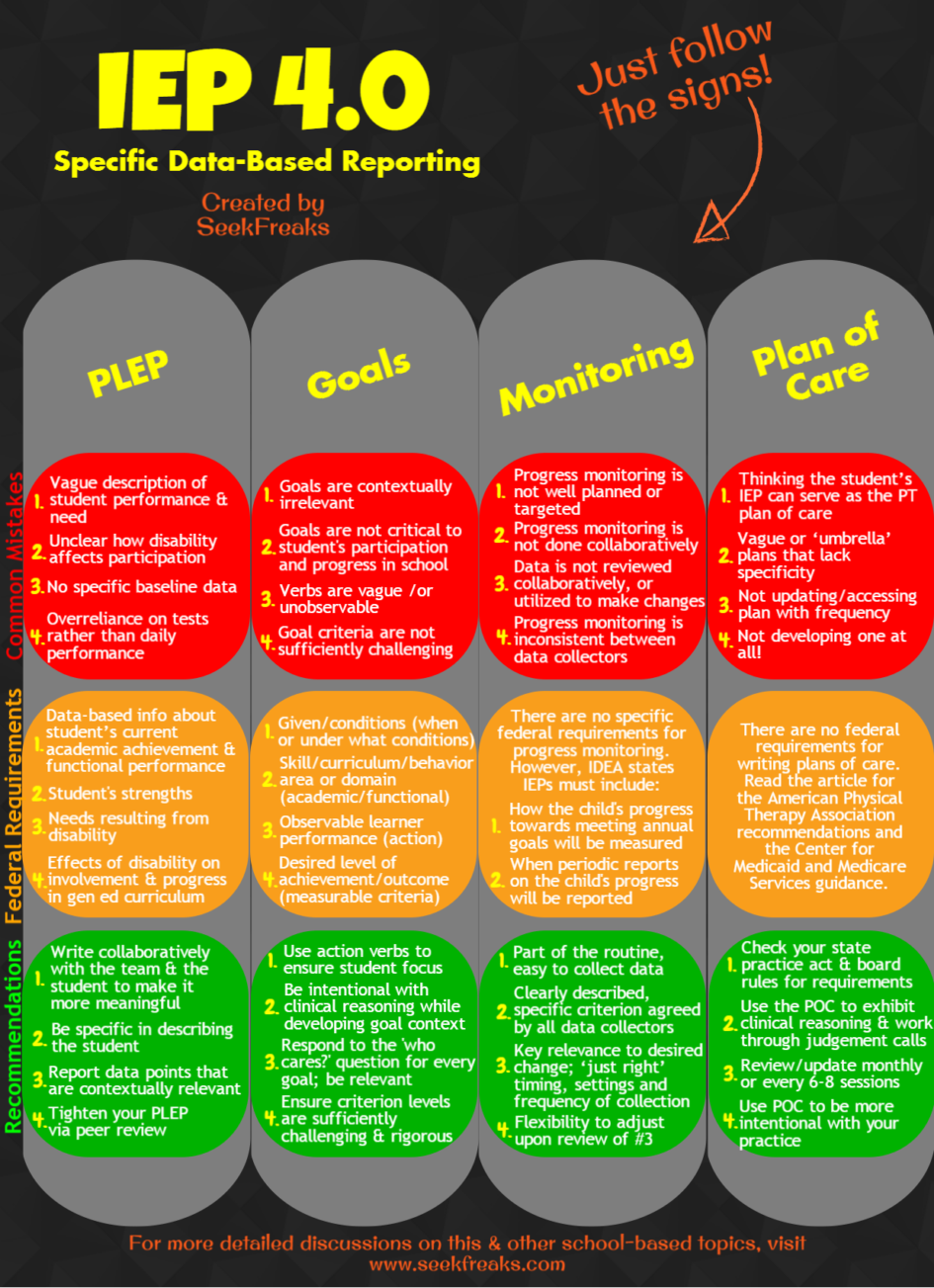
We have now reached the 4th and last installment of our IEP 4.0 series. While the first 3 focused on elements found in an IEP, the Plan of Care is not. But it should still be based on the contents of the IEP, so if you have not read the first 3 articles read them first:
- Developing a Clear Present Level of Performance
- Data-based and Student-focused Goals
- Collaborative Progress Monitoring
If you have read them, let’s go work on the plan of care…
A Plan of Care (PoC) is a document that identifies goals for the student and serves to guide our interventions. Most state OTand PT practice acts require a plan of care be written for each student receiving OT or PT, however, specifics can be hard to come by. As a first step, check out the language included in your state OT or PT practice act and Board Rules regarding PoCs. Are there specific requirements? Any details or guidance? Generally, state acts will require each individual receiving OT or PT services have an established plan of care or plan of intervention but do not specify anything!
The PoC can be a critical tool for our practice if we use it appropriately. PoCs should be full of our clinical reasoning and individualized to the specific student and circumstance.
This is where we do not collaborate – not on this one! The plan of care is written after we collaborate with the team to develop the Individualized Education Program (IEP). This plan is the occupational/physical therapist response to the IEP; how the OT and PT plans to intervene and contribute to the student attaining the established goals.
Many OTs and PTs believe, as do some Medicaid offices, that the IEP can serve as the OT/PT PoC. While the IEP does contain some of the elements, it does not provide all the detail needed from a PoC. Since there are no federal requirements for a PoC, we are relying heavily on APTA recommendations and guidance from the Centers for Medicare & Medicaid Services (CMS).
American Physical Therapy Association (APTA)
The APTA recommends that a plan of care be created for each individual receiving services to describe the therapist’s intentions. Here are the APTA Plan of Care Elements:
- Goals stated in measurable terms that indicate the predicted level of improvement in function
- Statement of interventions to be used; whether a PTA will provide some interventions
- Proposed duration and frequency of service required to reach the goals (# of visits per week, # of weeks, etc)
- Anticipated discharge plans
Centers for Medicare & Medicaid Services (CMS)
CMS is a bit more specific. CMS asserts that:
- provided services must directly and specifically relate to a written treatment or intervention plan
- the PoC must be:
- established by the PT who will provide the services
- signed with professional identification (OTR/L, PT, MSPT, DPT, etc.) and
- dated
- the PoC must include:
- diagnosis, including OT/PT diagnosis
- long term treatment goals
- type and amount of therapy interventions
- duration and frequency of therapy services (42CFR424.24, 42CFR424.27, 410.105 and 410.61)
SeekFreaks Recommendations
Clearly the IEP has goals, hopefully measurable goals as well as the duration and frequency of services. However, it does not include (and should not include!) any interventions or discharge plans. The IEP should be focused on student goals, not interventions. Student goals are functional and target the participation or activity levels of the International Classification of Functioning, Disability and Health (ICF). So if there are impairment level goals that need to be addressed they can be included in the PoC.
Also, if you are still sorting out the underlying issue, that can be included in the PoC. For example, Laurie has a balance impairment but you are not certain if it is caused by a strength limitation, proprioceptive impairment, neuromuscular delay or sensory issue. The PoC can be used to describe your clinical impressions, needed data and order of interventions to confirm your hypothesis.
Additionally, it is a great place to record your OT/PT ‘to-do’ list: who you need to follow up/communicate with, equipment you need to check, data you need to collect or other items you may forget.
Clinical reasoning belongs here and can help the itinerant OT/PT be intentional with your practice = flesh out interventions, delineate order of interventions, envision what discharge will look like. By doing so, the PoC can serve as a huge assist to improving your daily practice.
Too often, school-based OT/PTs either don’t write PoCs or have such cursory PoCs that they are not a good investment of time. It follows if the PoC is vague or lacks currency, soon it will be left behind and/or seen as busy work. If the PoC is frequently reviewed and updated, it can be a great tool on which busy OT/PTs, moving from school to school, can rely.
I would suggest including the student IEP goals on the PoC and then make the PoC the document you carry with you to track your service delivery. It is all yours, write in it what you will! As always, keep in mind that any document, scrap of paper or note can be subpoenaed.
Hopefully, you are moved to consider relying more heavily on your PoCs.
By the way, you just completed the series and the full infographic. It is time to print it out and place it where you typically complete your documentation.
~~~~~~~~~~0~~~~~~~~~~
References and Resources-
APTA Defensible Documentation. Documentation Checklist Sample: http://www.apta.org/Documentation/DefensibleDocumentation/
Centers for Medicare & Medicaid Services, Office of Financial Management. https://www.cms.gov/Research-Statistics-Data-and-Systems/Monitoring-Programs/Medical-Review/Downloads/TherapyCapSlidesv10_09052012.pdf
Join author, Laurie Ray, and her colleagues in the following continuing education courses…















May 6, 2016 at 5:42 am
Hi Laurie,
Thank you for another great series. I have been using my quarterly progress reports as plan of care and updating it thereafter in each contact note. I have created data tracking sheets for PE teachers who provide APE with consultation notes from me that can help them with their students. These are updated monthly. I think this last document is closer to what you describe. I am happy to revisit how I document and plan my services. What frequency is recommended for “officially” updating the plan of care if not as an ongoing basis with each visit?
May 6, 2016 at 2:13 pm
You should check your state’s PT practice act to see if a Plan of Care review cycle is specified. If not, I suggest at least revising it annually with the IEP review. I would recommend review and revision at each quarter or with the progress report. Many review and revise PoCs each month. It can vary greatly depending on your student, where you are in intervention and how much change/progress is occurring/anticipated.
I would love to see your data tracking sheets!! I think solutions like yours are the most sustainable. Whenever we can incorporate into current structures or achieve two objectives with one documentation=Huzzah!!
Thanks for the comment and suggestions!